Many people experiencing COVID vaccine cost confusion due to delay in insurance coding
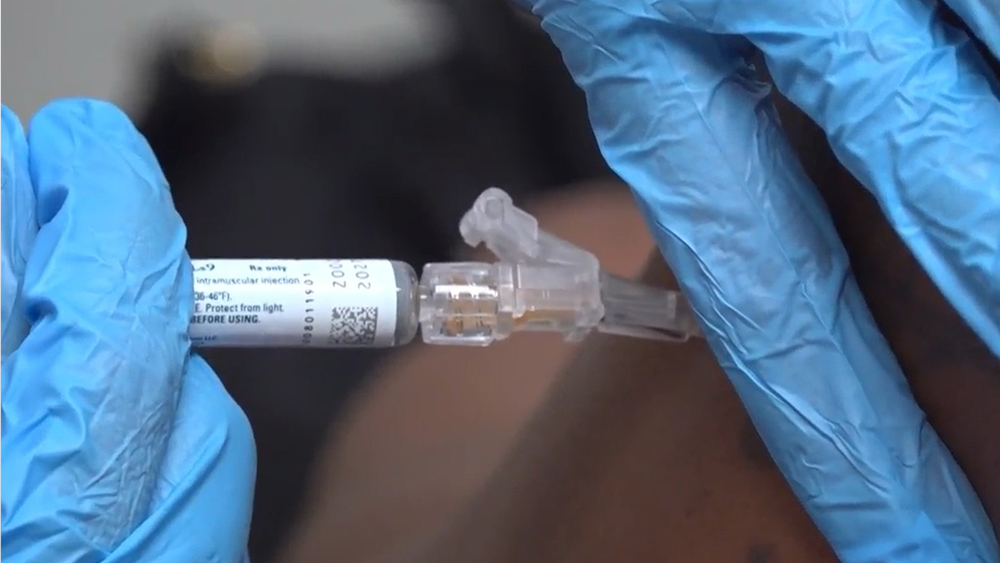
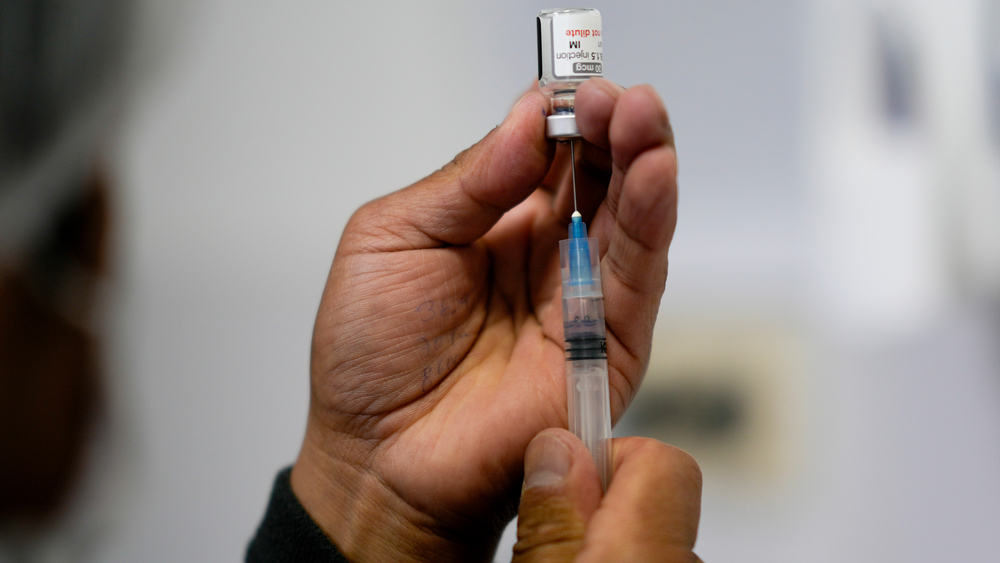
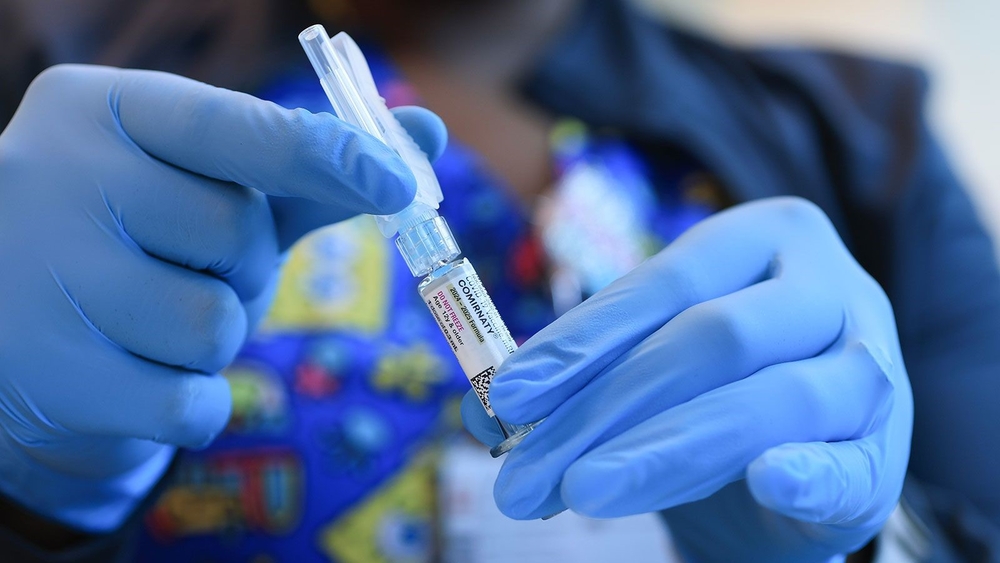
PHILADELPHIA -- As Americans roll up their sleeves to get the latest COVID booster, some are being asked to pay out of pocket.
Social media is erupting about over this issue.
"Trying to get my COVID booster this month and my insurance won't cover it. So that's fun," one post read.
"PSA: despite having an appointment, despite being in the right place at the right time, despite having insurance, I was not able to get my COVID booster today," read another.
To help sort out this mess, Action News reached out to the insurance companies, the pharmacies, and the federal government.
The Troubleshooters received an email on Thursday that read: "My son went (to CVS) for his COVID booster on Saturday and was turned away, telling him that he would have to pay $200."
Action News asked the U.S. Assistant Secretary for Preparedness and Response Dawn O'Connell about insurance not paying for the vaccine yet.
"Well, the insurers are responsible for covering the new costs, the costs associated with the new vaccine. The department's working closely with insurers and with the pharmacies to make sure that the little glitches we're starting to see are being smoothed out as quickly as possible," said O'Connell.
The Troubleshooters reached out to insurance companies and pharmacies, and some are pointing the finger of blame at each other.
For instance, CVS replied, "Some payers (meaning insurance companies) are still updating their systems... If this happens, our pharmacy teams can help patients schedule an appointment for a later date."
CIGNA Healthcare said it updated its systems with the new codes almost two weeks ago, but some pharmacies are submitting claims incorrectly.
Independence Blue Cross said, "We are aware of the unexpected delay in coding. As of Tuesday, September 19, the delay has been addressed and pharmacies are able to bill Independence directly."
The bottom line is your COVID boosters should be covered. If your claim is denied at the pharmacy, contact your insurer for reimbursement and make sure you're at a pharmacy covered by your plan.
"We want to make sure you're going to an in network provider to get your vaccine, and that'll smooth some of this over as we go," said O'Connell.
There is also a bridge program for those who are underinsured or uninsured.
You can also order free COVID test kits from the government beginning on Monday, September 25.
The kits will start shipping out a week later.
Independence Blue Cross Statement
Dr. Richard Snyder, Vice President of Facilitated Health Networks
We know that COVID-19 vaccines and booster shots are important tools that help reduce the risk of severe disease, hospitalization, and death. That's why the COVID-19 vaccine and booster shots are covered for Independence Blue Cross individual and group commercial members at no cost when they are obtained from an in-network provider or pharmacy. If COVID-19 vaccine or booster shots are administered by an out-of-network provider or pharmacy, standard cost sharing will be applied based on a member's health plan benefits. We recommend that members check their benefits to confirm in-network providers and if they have out-of-network coverage.
For Medicare Advantage members, coverage of the COVID-19 vaccine and booster shots are covered as a preventive service under Part B. For CHIP members, coverage of COVID-19 vaccine and booster shots are covered at no cost as a preventive service.
We are aware of the unexpected delay in coding to allow payment for the updated COVID-19 vaccine, which has resulted in some members being told the vaccine is not covered by their health insurance. This is something that is impacting most health insurers that are covering the vaccine. As of Tuesday, September 19, the delay has been addressed by the appropriate parties and pharmacies are able to bill Independence for the pharmacy benefit directly.
Independence members who paid out of pocket for the vaccine can request reimbursement.
Cigna Healthcare Statement
COVID vaccines are covered at no cost at any in-network pharmacy or doctor's office for Cigna Healthcare customers.
Rite Aid Statement
The new COVID-19 vaccine is expected to be in stores by this weekend. Customers can schedule appointments through our online scheduler at riteaid.com/pharmacy/scheduler or walk-in to their local Rite Aid to see if the vaccine is available.
CVS Statement
Some payers are still updating their systems and may not yet be set up to cover the updated COVID-19 vaccines. If this happens, our pharmacy teams can help patients schedule an appointment for a later date.
America's Health Insurance Plans Statement
The U.S. Food and Drug Administration (FDA) recently approved and the Centers for Disease Control and Prevention (CDC) recommended updated COVID-19 vaccines for everyone 6 months and older. Health insurance providers recognize the importance of these vaccines and continue to encourage everyone to get a COVID-19 vaccine.
AHIP members are covering the new COVID-19 shots with no cost sharing when obtained through a network provider. We are working closely with the federal government, pharmacies, and other partners to quickly ensure patient access to COVID-19 vaccines with $0 cost sharing and address any issues relating to newly added billing codes quickly.
Walgreens Statement
We are committed to ensuring no patient pays and everyone who is eligible and wants a vaccine receives one. COVID-19 vaccines will continue to be available at no cost to the public. The cost will either be covered by insurance or government assistance programs, such as the CDC's Bridge Access Program. Our pharmacists are aware of the procedures to process insurance claims and can assist those who have questions. We encourage everyone to bring insurance information to their appointment, if available, but will not turn away those whose insurance does not cover it.
Vaccinations for children aged 3-11 years will be available at select Walgreens locations as early as September 29. Appointments will be added on a rolling basis as this supply comes into our sites. Parents or guardians are highly encouraged to make appointments for this age group to ensure the best experience by visiting Walgreens.com/ScheduleVaccine, using the Walgreens app or calling 1-800-WALGREENS. We offer flexible openings, including nights, weekends and the ability to schedule multiple vaccines for multiple people in your family during the same visit.